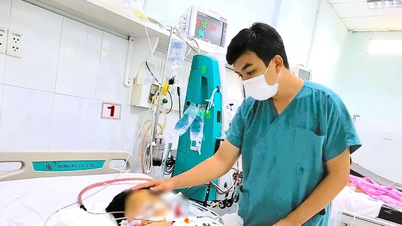
According to Dr. Nguyen Minh Quan (Hung Vuong Hospital) , on November 26, baby NLH, after 97 days of continuous treatment at the Neonatal Intensive Care Unit (NICU) and the Neonatal Department, reached 1,745 grams and was eligible to be discharged home.
Baby H. was born extremely prematurely at 23 weeks, weighing 640 grams. This is the smallest newborn baby ever successfully raised at the hospital.
The 23rd week of pregnancy is considered the "limit of survival" in obstetrics and pediatrics. At this stage, the lungs have almost no Surfactant production, the brain is prone to bleeding, the skin is paper-thin, and the immune system is not yet fully developed. Weighing only the equivalent of a large carton of fresh milk, baby H. faces the risk of severe respiratory failure, hypothermia, infection, and brain hemorrhage immediately after birth.
The baby was delivered naturally by his mother at 11:20 p.m. on August 21. Upon birth, his cyanosis, poor tone, and weak reflexes forced the team to actively resuscitate him in the delivery room: keeping him warm, intubating him, using a ventilator, and continuously monitoring his vital signs. After initial stabilization, the baby was transferred directly to the NICU.
Upon admission to the NICU, the baby was placed on surfactant and invasive mechanical ventilation, which improved his oxygen saturation and skin color. He remained on the ventilator for 55 days, a period that required delicate adjustments to minimize lung damage. He was then switched to high-flow nasal cannula (HFNC) for another 18 days.

Baby H. was discharged from the hospital on November 26, after 97 stressful days, to the joy of her family and many medical staff at Hung Vuong Hospital.
For nearly two months, baby H. underwent many rounds of treatment for sepsis with strong antibiotics, blood transfusions for anemia, and vasopressors to maintain blood pressure. On the 58th day after birth (October 17), the baby reached 1,180 grams, an important milestone that allowed him to be transferred to the Neonatal Department for recovery.
Despite her weak respiratory capacity, the baby continued to be monitored for apnea, treated with antibiotics and given respiratory physiotherapy. Kangaroo care (direct skin-to-skin contact with the mother or caregiver’s bare chest) was regularly used to help stabilize body temperature, breathing rate and enhance mother-child bonding.
Nutrition begins with breast milk through a tube, then the baby learns to eat with a spoon and progresses to breastfeeding, a sign that the baby has matured neurologically and can coordinate the sucking - swallowing - breathing reflexes.
Dr. Le Anh Thi, Head of NICU at Hung Vuong Hospital, said that keeping a baby alive at 23 weeks requires standardization of procedures from resuscitation in the delivery room, intubation, timely Surfactant injection, to continuous low-dose ventilator operation. Incubator systems, high-frequency ventilators, and specialized drugs help create an optimal environment for extremely premature babies to have a chance to survive.
"In addition to expertise, family support plays a key role. Regularly providing breast milk and daily Kangaroo care helps babies stabilize better, reduces the risk of infection, and promotes weight gain," Dr. Thi added.
According to the expert, the successful case marks a major step forward in neonatal care in Vietnam, bringing Hung Vuong Hospital closer to the treatment standards of international pediatric centers for extremely premature infants. Baby H., from a 640 gram life, is now leaving the hospital healthy, opening up hope for many other high-risk cases.
Source: https://suckhoedoisong.vn/ky-tich-nuoi-song-be-sinh-non-23-tuan-nang-640g-o-tphcm-169251128130331227.htm










































































































Comment (0)