Underbite, also known as reverse bite, is a relatively common pathological condition involving abnormal jaw position and size, particularly in Southeast Asia, with a prevalence rate of 4 to 6.5%.
Causes and symptoms
In patients with underbite, the most common sign is that the lower incisors are positioned further forward than the upper incisors. Patients may also notice a protruding chin and a recessed upper jaw. In severe cases, the face may appear plow-shaped or crescent-shaped, as it is commonly called.
Underbite can be caused by the upper jaw being recessed, the lower jaw being protruded, or both. Common causes include genetics, trauma, tumors that alter jaw size, and craniofacial syndromes (Crouzon, Apert, Pfeiffer...).
There is no evidence to suggest that habits such as chewing excessively on one side or lying on one side have an impact on the jawbone. Underbite patterns can develop from childhood or during puberty, so some patients may have a normal face in childhood but experience significant changes leading to an underbite during puberty.
Signs of an underbite include the upper incisors being behind the lower incisors (normally the upper incisors are 2 to 4 mm ahead of the lower incisors); the mid-face is flat, lacking convexity, and the nasolabial folds may be concave; the chin protrudes forward and may be lệch to one side, and the patient may have a "plow-shaped" or "crescent moon" facial shape similar to the description of a witch's face in Western literature.
This cosmetic defect is difficult to correct with camouflage treatments such as orthodontics, fillers, or Botox and negatively impacts a patient's life opportunities and self-confidence. The lower incisors tend to protrude in front of the upper incisors.
In severe cases, the front teeth of both jaws may not touch each other, making eating difficult and preventing the patient from biting through food with their front teeth. Speech can also be severely affected, as teeth and lips are part of the vocal apparatus. When the teeth and lips are not in harmony (they don't touch), some sounds, such as /f/ or /v/, may be difficult to pronounce, potentially leading to speech impediments.
Crowded and misaligned teeth, with lower incisors either pointing straight up or tilted backward, creating small gaps that are difficult to clean, and thin alveolar bone (the bone surrounding the tooth roots) make teeth more prone to falling out in old age.
Combined treatment involves jaw surgery and orthodontic treatment.
In terms of treatment, during the period when children are losing their baby teeth, dentists can have them wear a facemask appliance to pull the upper jaw forward with a success rate of 75%; however, this method is only effective for the upper jaw, and appliances that intervene in the lower jaw are almost ineffective.
Once puberty is over, there are two main treatment options: one is invisible orthodontics, and the other is a combination of jaw surgery and orthodontics (also known as teeth straightening or braces).
Concealed orthodontics means using tooth movement to try to mask jaw misalignments. Orthodontists may use techniques to make the upper teeth overlap the lower teeth.
In most cases, this method can make the patient's teeth look almost normal, but the overall facial appearance remains unchanged and may even worsen because the upper incisors protrude further forward and the lower incisors tilt further backward (which already had a tendency to tilt). This can even damage the alveolar bone, increasing the risk of lower incisors falling out in the long term.
Orthodontic surgery combined with jaw correction is the most thorough and effective treatment method for cases of underbite (reverse bite). Underbite, and dental and facial deformities in general, are caused by misalignment of the jawbone in terms of position and size. Therefore, the teeth erupting from the bone will change position and angle in an attempt to adapt to the incorrect jawbone position.
Therefore, the treatment process needs to include two components: surgery to reposition the jawbone to its proper size and position, and orthodontics to adjust the teeth to fit together in their new jawbone position. It is important to emphasize that, in the vast majority of cases, the combination of orthodontics and surgery is essential to achieve the best aesthetic and functional results.
The surgery is typically performed after puberty, usually at age 15 for girls and 17 for boys. Depending on professional requirements, time constraints, and patient preferences, the doctor may perform orthodontic treatment first, then surgery, or surgery first, then orthodontic treatment.
The orthodontic-first, surgical-later sequence is the traditional approach, still widely used today due to its high accuracy and ease of surgical execution, and can be applied to most cases.
In this treatment plan, the orthodontist will first intervene to reposition the misaligned teeth, straighten crowded teeth, and return them to their correct positions on the dental arch. This process will take approximately 6 months to 1.5 years, depending on the complexity and whether or not tooth extraction is required.
After the preparation phase is complete, the patient will undergo orthodontic surgery. Two weeks after the surgery, the patient will have further orthodontic treatment to perfect the bite over approximately six months. If all steps go smoothly, the total treatment time will last about two years. The disadvantage of this protocol is the long waiting time before surgery.
During orthodontic treatment in preparation for surgery, patients' appearance and function may even deteriorate compared to before treatment, leading to a decrease in their morale and quality of life.
In the surgical-pre-orthodontic sequence, the patient undergoes jaw bone repositioning first, followed by orthodontic treatment to realign the teeth to their correct positions. The disadvantage of this method is that the accuracy is slightly reduced compared to the traditional treatment sequence, and the surgery is more complex for the surgeon.
However, this protocol is superior in terms of time and provides a better patient experience due to immediate aesthetic improvements. Thanks to the accelerated orthodontic effect when the body starts its healing process after surgery, the time it takes for teeth to move after the operation is also significantly shortened.
The total treatment time can be significantly shortened to 9 months to 1 year under ideal conditions and with the patient adhering to the doctor's instructions. In some difficult cases, where teeth cannot be moved as desired by the doctor, surgery first followed by orthodontics is the necessary option.
Surgical techniques for correcting malocclusion and post-operative care.
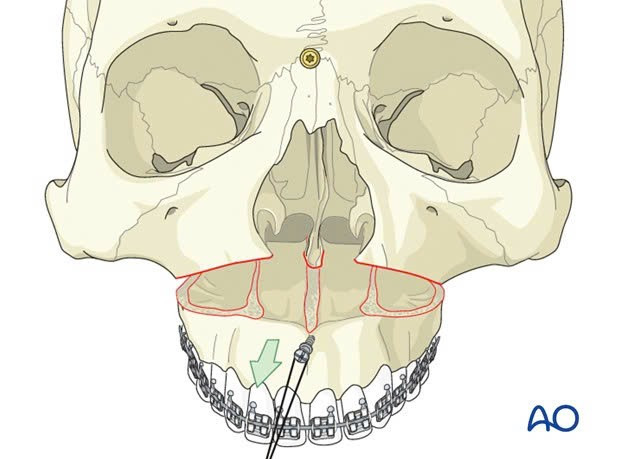
There are three main techniques used in orthognathic surgery to correct underbite. For the upper jaw, the Le Fort I osteotomy technique is the most common method to separate the upper jaw's tooth-bearing portion and move it in three dimensions into a predetermined position.
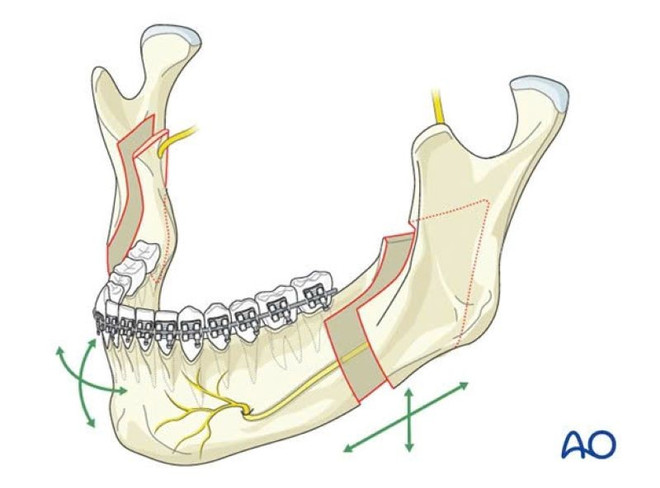
For the lower jaw, surgeons often use the technique of splitting the mandibular ramus (Bilateral sagittal split osteotomy - BSSO) to move the jawbone into the desired position. Chin reshaping can be performed simultaneously with double jaw surgery to achieve a more harmonious facial appearance; in this technique, the chin bone is separated and moved in three dimensions to the appropriate position.
Currently, orthognathic surgery to treat underbite has become a routine procedure, with each surgery lasting only 2 to 4 hours instead of 6 to 8 hours as before. The hospital stay has also been reduced to only 2 to 3 days.
During the post-operative period, patients experience very little pain, which can be easily controlled with common painkillers. Patients can return to school or work 1-2 weeks after surgery; they can eat and drink normally after 6 weeks; and swelling will completely subside after 6 months. Patients may experience mild numbness in the upper and lower lips, which usually disappears after a few months.
Application of 3D technology in jaw surgery.
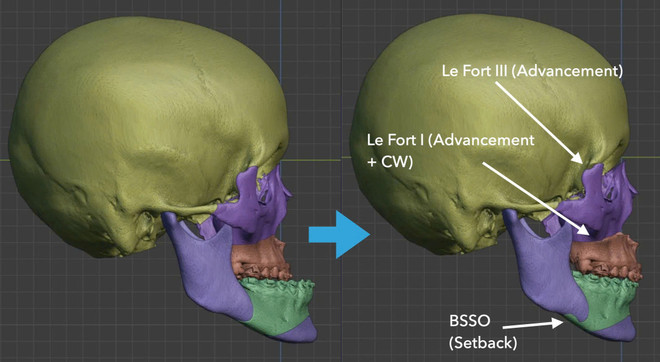
Today, with specialized software and high-resolution CT scans, doctors can accurately calculate the degree of misalignment in patients to determine the most appropriate treatment plan. The movement of the jawbone is calculated with millimeter precision.
Personalized surgical guidance tools for each patient are also designed on the computer and used to guide surgeons during the operation.
Patients in Vietnam can access these technologies just as they do in developed countries around the world .
Source: https://www.vietnamplus.vn/phuong-method-treatment-hamstring-redness-post1061231.vnp



![[Image] Bridges and roads connecting the eastern part of Ho Chi Minh City](https://vphoto.vietnam.vn/thumb/1200x675/vietnam/resource/IMAGE/2026/04/16/1776328595108_ndo_br_bh-vt5-jpg.webp)

































































![[Infographic] Details of the Hanoi-Quang Ninh High-Speed Railway Project](https://vphoto.vietnam.vn/thumb/402x226/vietnam/resource/IMAGE/2026/04/16/1776338188424_anh-man-hinh-2026-04-16-luc-18-16-10.png)
![[Photo] National Assembly Chairman Tran Thanh Man meets with the Speaker of the Georgian Parliament](https://vphoto.vietnam.vn/thumb/402x226/vietnam/resource/IMAGE/2026/04/16/1776338494029_anh-man-hinh-2026-04-16-luc-18-21-21.png)

































Comment (0)