Dr. Nguyen Thanh Khiem, from the Department of Gastrointestinal, Hepatobiliary, and Pancreatic Surgery at Bach Mai Hospital, shared his insights regarding patients with bile duct cancer.
Accordingly, this type of malignant cancer can arise from any component of the bile ducts (most commonly, accounting for 95%, originating from the bile duct epithelium).
Biliary tract cancer accounts for 2% of gastrointestinal cancers and is classified as intrahepatic biliary tract cancer (accounting for 20%) or extrahepatic biliary tract cancer (accounting for 80%).
Currently, advanced techniques in treating liver and biliary tract diseases have significantly extended the lives of patients (image source: Bach Mai Hospital).
Extrahepatic bile duct cancers include hilar cholangiocarcinoma (Klatskin tumor) and cholangiocarcinoma of the common bile duct.
Klatskin tumors are the most common type of cholangiocarcinoma, accounting for 50-60% of all cholangiocarcinomas. Klatskin tumors are defined as cholangiocarcinomas located within 2 cm of the common hepatic duct branching point.
Regarding the prognosis for Klaskin tumors, the overall 5-year survival rate for patients who undergo radical surgery is 20-30%, depending on the study; however, for patients who are not candidates for radical surgery, this rate is 0%.
Therefore, despite being a highly aggressive type of cancer, radical surgery significantly improves the prognosis for patients.
Advanced Klaskin tumors with upward vertical spread, defined as Klaskin tumor type IV according to the Bismuth classification system, are cases of hilar arteriovenous malformations where the tumor has invaded the intrahepatic right and left hepatic ducts.
Previously, type IV Klaskin tumors were classified as unresectable, and the surgical choice was often hepatorenal anastomosis, a palliative surgery that did not remove the tumor, resulting in a very poor prognosis for post-operative survival.
However, with the continuous development of surgical techniques and multidisciplinary collaboration (Anesthesiology, Oncology, and Interventional Radiology), radical surgical methods for type IV Klaskin tumors have been successfully implemented at several major hepatobiliary surgery centers worldwide .
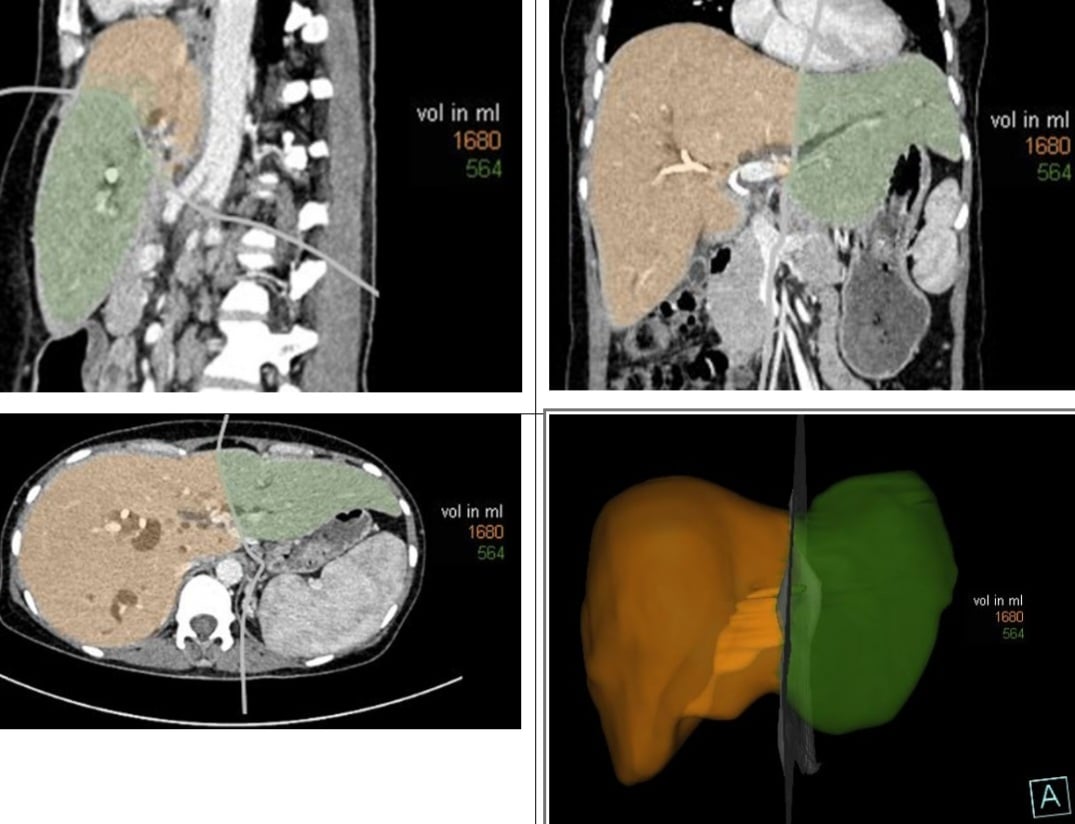
The diagram shows the planned liver resection (in orange). All cases underwent preoperative imaging, reconstruction, and liver volume measurement. This helped the surgical team plan the liver resection, estimate the percentage of liver to be removed, and determine the remaining liver volume, thereby developing an appropriate surgical strategy.
As a major center for hepatobiliary and pancreatic surgery, the Department of Gastrointestinal, Hepatobiliary, and Pancreatic Surgery at Bach Mai Hospital has successfully received and performed radical surgery on many patients with type IV Klaskin tumors.
In these cases, the Neuhaus procedure – a major liver resection technique – is now performed, including resection of the right lobe and the entire first subsegment, resection of the biliary bifurcation to the lateral segmental hepatic duct, and dissection of the celiac pedicle lymph nodes. The hilar tumor is resected along with the above components as a single block (en bloc) using a no-touch technique, contributing to curative treatment efficacy and oncological criteria (immediate intraoperative biopsy of the remaining hepatic duct and common bile duct is negative).
However, this is also a complex liver resection technique, with the volume of liver removed relatively often accounting for about 81% of the total liver volume according to studies. Therefore, the most common risk, and also the highest risk of postoperative mortality, is postoperative liver failure due to insufficient remaining liver volume.
Therefore, to minimize the risk of postoperative liver failure, meticulous perioperative management and accurate assessment of the function of the remaining liver are crucial.
Several interventions have been widely accepted to reduce the risk of hepatic failure after hepatectomy, including preoperative biliary drainage and portal vein embolization to increase the volume of remaining liver tissue. These meticulous surgical preparations are crucial to avoiding hepatic failure after hepatectomy.
In cases where patients undergo percutaneous biliary drainage 3 weeks prior to surgery, multislice computed tomography with reconstruction and liver volume measurement are routinely performed to accurately calculate liver volume and improve liver quality before surgery.
Source











































































![[Image] Close-up view of the 10-lane road connecting to Long Thanh Airport](https://vphoto.vietnam.vn/thumb/402x226/vietnam/resource/IMAGE/2026/04/04/1775291871988_ndo_br_1-resize-5690-jpg.webp)

































Comment (0)